We are often asked “are stair lifts covered by Medicaid?” Yes, stair lifts are covered by Medicaid for qualified individuals through Home & Community Based Services or HCBS Waivers. While coverage depends on your state and Medicaid eligibility, many state Medicaid programs will pay for part or all of the cost to install a stair lift in your home through their waiver programs.
Understanding the eligibility for a waiver program can be quite complex. Below, we go into detail on some of the requirements that must be met when seeking Medicaid coverage of a stair lift.
Navigating Eligibility for a Stair Lift Covered by Medicaid
Eligibility for Regular Medicaid
Level of Care Required
Waiver Programs
- Financing

If you are already Medicaid waiver approved and would like to speak to an Options HME Stair Lifts representative about having a stair lift installed in your home, please contact us. If you would like to know whether Medicare covers stair lifts, please visit our page: Are Stair Lifts Covered by Medicare?
Since Options HME Stair Lifts serves Southern Illinois and the St. Louis, Missouri area, we will focus on the state Medicaid requirements as they apply in Illinois and Missouri. However, many states use similar requirements and programs.
Medicaid Eligibility
To qualify for a waiver program, an individual must first be eligible for their State Medicaid coverage.
Illinois – Some residents may qualify for Medicaid coverage based on income alone. This is typically determined by whether the household’s annual income falls below a set percentage of the Federal Poverty Level. Some Illinois residents can also qualify for Medicaid coverage on the basis of family status, disability, or age. For more information, visit: Illinois State Medicaid Website.
Missouri – In Missouri, it is unlikely that residents will qualify for Medicaid coverage just on the basis of household income. Instead, coverage is typically extended on the basis of family status, disability, or age, where the household or individual is ALSO low income. For more information, visit: Missouri State Medicaid Website
In both states, Medicaid eligibility alone is not sufficient to provide coverage for a stair lift. Illinois and Missouri each provide funding for stair lifts through waiver programs. For information regarding Medicaid in general, visit the United States Government Medicaid site: medicaid.gov.
Level of Care Required
To be eligible for a waiver, the recipient must meet the “Level of Care Required” threshold. Level of Care Required means that an individual must be eligible to receive a specific level of care through regular Medicaid to utilize a waiver program. For instance, someone who receives Medicaid but is capable of living with their family or on their own, often does not meet the required level of care. However, a disabled individual who is unable to remain at home due to a disability or worsening health would be deemed “Nursing Home Eligible” or “Eligible for Institutional Level of Care.” If equipment such as a stair lift or skilled home care allows the individual to remain at home, they are likely eligible for a waiver.
HCBS Waiver Programs
The state’s waiver programs are where Medicaid recipients will find coverage for a stair lift. Each state maintains their own set of waiver programs aimed at providing assistance for those eligible. The waivers are provided through Home and Community Based Services, whose aim is to “provide opportunities for Medicaid beneficiaries to receive services in their own home or community rather than institutions or other isolated settings” (medicaid.gov). Essentially a waiver allows the recipient or their family to waive an aspect of their Medicaid care, in favor of receiving the benefit in a different way. Waiver programs give Medicaid recipients a choice as to how to receive their Medicaid coverage, without compromising future benefits.
For example, an individual eligible for Medicaid covered nursing home care can utilize a waiver program to pay for the cost of a stair lift, if that lift is necessary to allow them to continue living in their own home. Or the parents of a disabled child may opt to utilize a waiver program in order to install a stair lift for their child. It allows the child to continue living with their family instead of moving the child to a nursing care facility.
Illinois Medicaid Waivers
Illinois maintains the following nine waiver programs, operated by five Operating Agencies. Contact the Operating Agency listed for more information about a waiver program you are enrolled in or believe you may be eligible for. More information about the waiver programs can be found at the Illinois HCBS Waiver Site.
Division of Developmental Disabilities (DDD) – 1-888-337-5267
Adults with Developmental Disabilities Waiver
Residential Services for Children and Young Adults with Developmental Disabilities Waiver
Support Waiver for Children and Young Adults with Developmental Disabilities Waiver
Division of Specialized Care for Children (DSCC) – 1-800-322-3722
Medically Fragile/Technology Dependent Children Waiver
Department on Aging (DoA) – 1-800-252-8966
Persons who are Elderly Waiver
Division of Rehabilitation Services (DHS-DRS) – 1-800-843-6154
Persons with Brain Injury (BI) Waiver
Persons with Disabilities Waiver
Persons with HIV or AIDS Waiver
Department of Healthcare and Family Services (HFS) – 217-782-0545
Supportive Living Program Waiver
Missouri Medicaid Waivers
Missouri’s Medicaid, also known as Mo HealthNet, maintains 12 waiver programs operated by two Operating Agencies. Contact the Operating Agency listed for more information about a waiver program you are enrolled in or believe you may be eligible for. For additional information about Missouri’s Medicaid waiver programs visit: Missouri Department of Social Services Site.
Department of Health & Senior Services (DHSS) – 573-751-6400
Adult Day Care Waiver
Aged and Disabled Waiver
AIDS Waiver
Brain Injury Waiver
Independent Living Waiver
Medically Fragile Adult Waiver
Structured Family Caregiving Waiver
Division of Developmental Disabilities (DDD) – 573-751-4054
MO Children with Developmental Disabilities (MOCDD) Waiver
Autism Waiver
Comprehensive Waiver
Community Support Waiver
Partnership for Hope Waiver
*Not every waiver on this list offers stair lift coverage, however which waiver best applies to your situation and which waiver offers the best chance at stair lift coverage is very dependent on each unique set of circumstances. Therefore, it is important to contact one of the operating agencies in order to determine which waiver best applies.
Less Expensive Alternatives
If you are unable to receive any funding through Medicaid, there are other options for reducing the cost of a stair lift. Options HME Stair Lifts gives you the option to purchase a stair lift new, used, or as a rental. Purchasing a used stair lift can often save $1000 or more. If purchasing is still too expensive or you believe you may only need the stair lift for a short period of time, renting is a great option. We offer stair lift rentals at a low monthly cost, with no long term contracts required. Contact us if you would like to know more about your options for purchasing or renting a stair lift.

Designed to make accessing your basement or second floor safe & easy.
Industry leading stair lifts with great warranties.
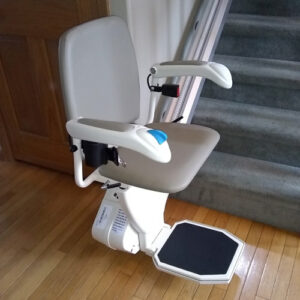
Used stair lifts offer the same great benefits, at a lower cost!
Every used stair lift undergoes a 35-point inspection and is backed by a 1 year parts & labor warranty.

An excellent short term solution while recovering from an injury or surgery.
Our stair lift rental is simple and affordable. No long term contracts, just an easy monthly payment.
Financing
If you are not covered by Medicaid or find the cost of a used stair lift difficult to cover, financing may be a great option. It allows you to break the cost of a stair lift into affordable monthly payments. Learn more about our financing options here.
